What the U.S “Advancing Global Health” Initiative Means for Africa’s Health Security and Sovereignty

Kenya Advances Public Health Emergency Response Systems through Validation of a Risk-Based Decision-Making Tool
February 20, 2026
Kenya Launches NAPHS II and KNPHI Strategic Plan to Strengthen Epidemic Intelligence and Digital Public Health Systems
March 28, 2026The Center for Global Health and Pandemic Intelligence (CGP) examines the strategic implications of the initiative for African governments, regional institutions, and research organizations.
Dr. Mark Nanyingi | Nairobi-Kenya| March 10, 2026- 23:00
The U.S. Department of State, through its Bureau of Global Health Security and Diplomacy (GHSD), has launched a major global funding initiative titled Advancing Global Health. Structured as an Annual Program Statement (APS) with rolling Addenda, the initiative establishes a flexible financing framework designed to support global health security priorities over the coming years. With award sizes ranging from USD 500,000 to USD 250 million, the program represents one of the most substantial diplomatic financing mechanisms currently available for strengthening pandemic preparedness, surveillance systems, and outbreak response capacity worldwide.
For African countries, the initiative arrives at a pivotal moment. Following the COVID-19 pandemic and successive outbreaks of Ebola, cholera, and Mpox, governments across the continent are accelerating efforts to modernize national health security systems and address structural vulnerabilities exposed by recent crises.
The initiative also intersects with the continental vision of Africa Health Security and Sovereignty (AHSS) championed by the Africa CDC. If strategically aligned with national preparedness priorities, the initiative could accelerate investments in surveillance modernization, outbreak intelligence systems, laboratory capacity, and emergency response infrastructure.
A New Diplomatic Financing Architecture for Global Health
The Advancing Global Health APS represents a shift from traditional project-based global health assistance toward a framework financing architecture. Instead of issuing isolated funding calls tied to narrowly defined project scopes, the APS establishes a multi-year umbrella mechanism through which targeted funding opportunities known as Addenda can be released in response to evolving global health priorities. This model offers several strategic advantages, it.
- Enables more adaptive financing, allowing investments to respond quickly to emerging disease threats and preparedness gaps.
- Strengthens the link between global health investments and diplomatic engagement, as U.S. embassies play a central role in identifying country-specific priorities in collaboration with national governments.
This approach reflects a broader evolution in global health diplomacy, where pandemic preparedness is increasingly viewed not only as a development priority but also as a strategic international security concern.
“The emergence of flexible financing mechanisms such as the Advancing Global Health initiative signals a shift in global health diplomacy—from reactive outbreak funding toward strategic investment in preparedness systems. For Africa, the critical task is ensuring these resources strengthen integrated epidemic intelligence architectures capable of translating surveillance data into rapid public health action.”
— Dr. Mark Nanyingi, Center for Global Health and Pandemic Intelligence (CGP)
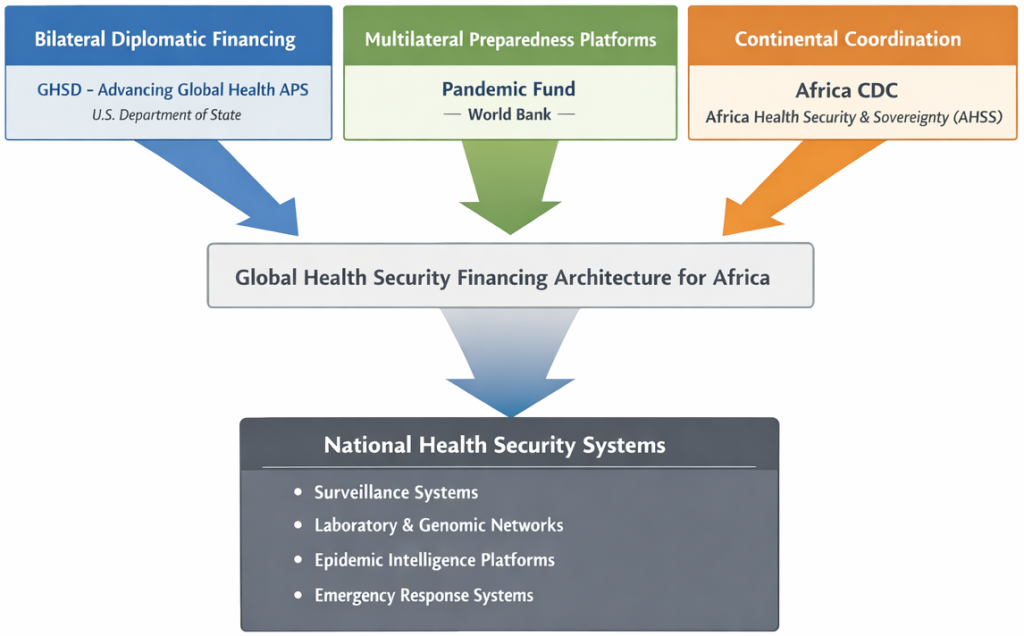
The Rapid Outbreak Response (ROR) alignment with 7-1-7
One of the most significant components of the initiative is the Rapid Outbreak Response (ROR) funding window. The ROR mechanism focuses on strengthening countries’ ability to detect outbreaks early and contain them rapidly, preventing localized health events from escalating into large-scale epidemics or pandemics. These priorities align closely with emerging operational benchmarks for outbreak detection and response, including the 7-1-7 target framework, which calls for detecting outbreaks within seven days, notifying public health authorities within one day, and initiating an effective response within seven days. Financing mechanisms such as the GHSD APS could play a critical role in enabling countries to operationalize these targets by strengthening surveillance systems, laboratory networks, and rapid response coordination mechanisms. Priority investment areas include:
- Integrated disease surveillance systems
- Laboratory diagnostics and genomic sequencing
- Field epidemiology and outbreak investigation capacity
- Emergency operations centers and incident management
- Coordination systems for rapid response teams
These priorities align closely with preparedness frameworks led by the World Health Organization under the International Health Regulations (2005). In this sense, the APS may function as a country-led implementation accelerator for IHR core capacities, enabling governments to operationalize priority gaps identified through national preparedness assessments while aligning investments with domestically defined health security strategies
Alignment with Africa’s Health Security and Sovereignty Agenda
The initiative also intersects with Africa’s evolving continental health security architecture. The Africa Centres for Disease Control and Prevention has articulated a strategic framework known as Africa Health Security and Sovereignty (AHSS), which aims to strengthen the continent’s capacity to prevent, detect, and respond to public health threats while reducing reliance on external systems.
The AHSS agenda emphasizes several core priorities:
- Strengthening surveillance and epidemic intelligence systems
- Expanding public health workforce capacity
- Increasing regional manufacturing of medical countermeasures
- Strengthening emergency preparedness and response infrastructure
The GHSD APS could complement these priorities by supporting country-level preparedness investments that feed into regional surveillance and response networks coordinated by Africa CDC. If aligned effectively, this financing mechanism could reinforce the broader AHSS objective of building a more autonomous and resilient African health security ecosystem capable of managing emerging threats with greater independence and coordination.E strengthens existing surveillance systems while reducing decision latency during escalation.
Opportunities for African Research and Innovation Institutions
Beyond governments, the initiative also opens new opportunities for African research institutions, technical organizations, and innovation hubs. Institutions capable of integrating scientific research, policy analysis, and operational implementation are likely to be particularly well positioned under the APS framework.
Priority areas of expertise may include:
- Epidemic intelligence platforms and analytics systems
- Genomic surveillance networks
- Atificial intelligence for outbreak detection and forecasting
- One Health surveillance systems
- Operational research on emergency response systems
Organizations that demonstrate regional collaboration, implementation capacity, and policy relevance may have a strategic advantage as countries develop proposals aligned with national preparedness priorities.s.
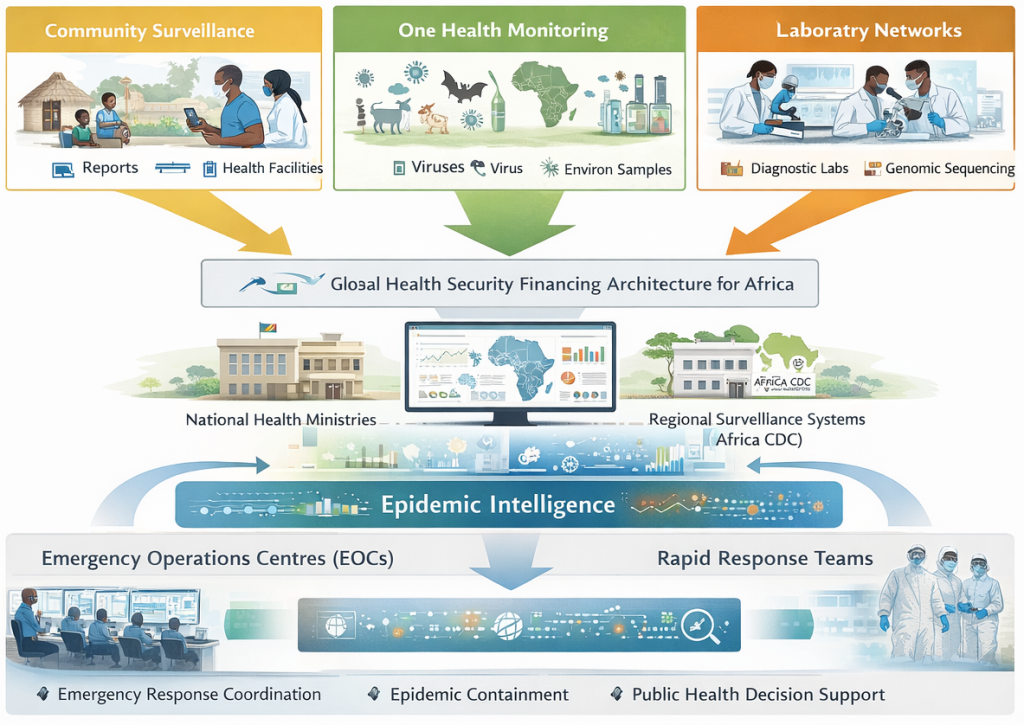
Policy Implications for Africa’s Epidemic Intelligence Architecture
The evolving global health security financing landscape shaped by initiatives such as the GHSD Advancing Global Health APS, the Pandemic Fund, and continental coordination under the Africa Centres for Disease Control and Prevention’s Africa Health Security and Sovereignty (AHSS) framework creates a strategic opportunity to strengthen Africa’s epidemic intelligence systems.
However, financing alone will not automatically translate into improved outbreak preparedness. To ensure that new investments generate measurable preparedness gains, several policy priorities warrant attention.
- African governments should prioritize the development of integrated epidemic intelligence platforms that consolidate data streams from surveillance systems, laboratories, environmental monitoring, and community reporting mechanisms into unified analytic environments.
- Investments in surveillance infrastructure must be complemented by advanced analytics capacity, including artificial intelligence, predictive modelling, and real-time risk assessment tools capable of translating data into actionable public health insights.
- Stronger institutional linkages between national public health institutes, emergency operations centres, and regional coordination platforms will be essential to ensure that analytic outputs inform operational decision-making during outbreaks.
- Strengthening epidemic intelligence ecosystems will require sustained investment in public health workforce development, particularly in data science, digital epidemiology, and epidemic intelligence analysis.
Institutions such as the Center for Global Health and Pandemic Intelligence (CGP) will play an important role in supporting this transition by advancing approaches that integrate surveillance data, analytic technologies, and decision-support tools within national and regional epidemic intelligence ecosystems


